Inpatient detox and rehab programs in Virginia provide structured, medically supervised care for individuals seeking treatment for substance use. Detox is typically the first phase, focusing on managing withdrawal symptoms and stabilizing the body in a safe clinical environment. After stabilization, inpatient rehab continues with a more comprehensive approach that includes therapy, behavioral support, and ongoing care planning.
In Virginia, treatment providers follow clinical and safety standards established by the Virginia Department of Behavioral Health and Developmental Services (DBHDS), which guide how detox and ongoing care are delivered. Individuals may also access community-based resources, such as Fairfax County Community Services Board substance use disorder programs, which offer local support services and recovery-focused care.
While detox is an important starting point, it is not considered complete treatment. Long-term recovery generally involves additional care that addresses the behavioral, psychological, and environmental factors associated with substance use.
The following key facts outline what to expect from inpatient detox and rehab in Virginia and how the recovery process typically progresses.
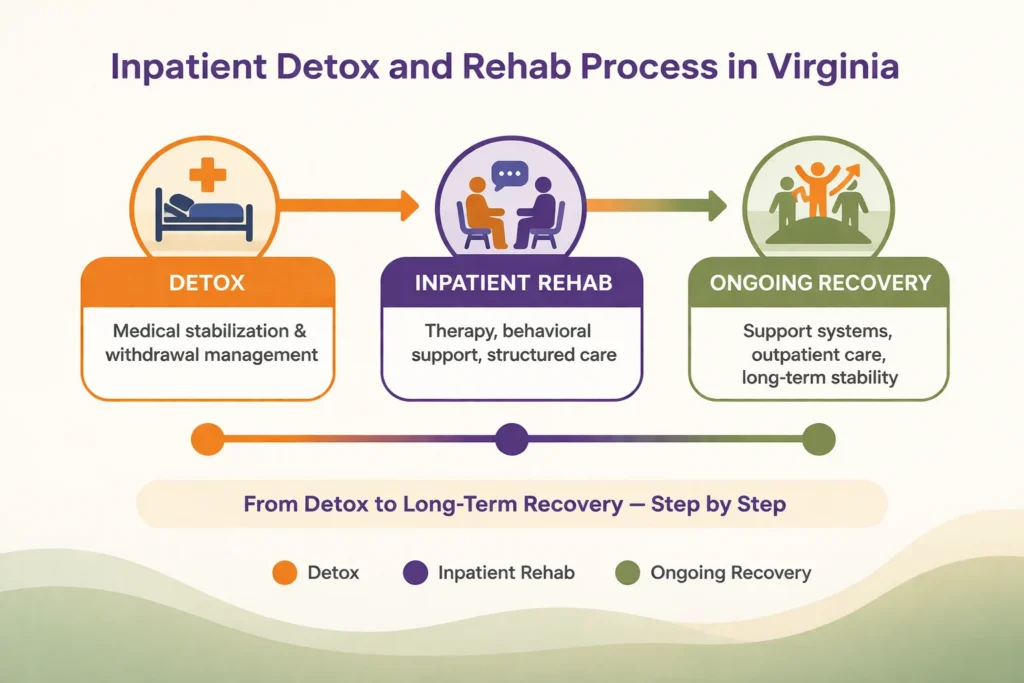
1. Detox Is the First Step, Not the Full Treatment
Detox is the initial phase of treatment, focused on safely managing withdrawal symptoms as the body adjusts to the absence of substances. This process is typically conducted under medical supervision to reduce health risks and support physical stabilization. While detox is an essential first step, it does not address the behavioral, psychological, or environmental factors associated with substance use.
For this reason, detox is often followed by ongoing care, which may include therapy, structured programs, and long-term support. Understanding the difference between detox and rehab helps clarify why continued treatment is considered an important part of recovery.

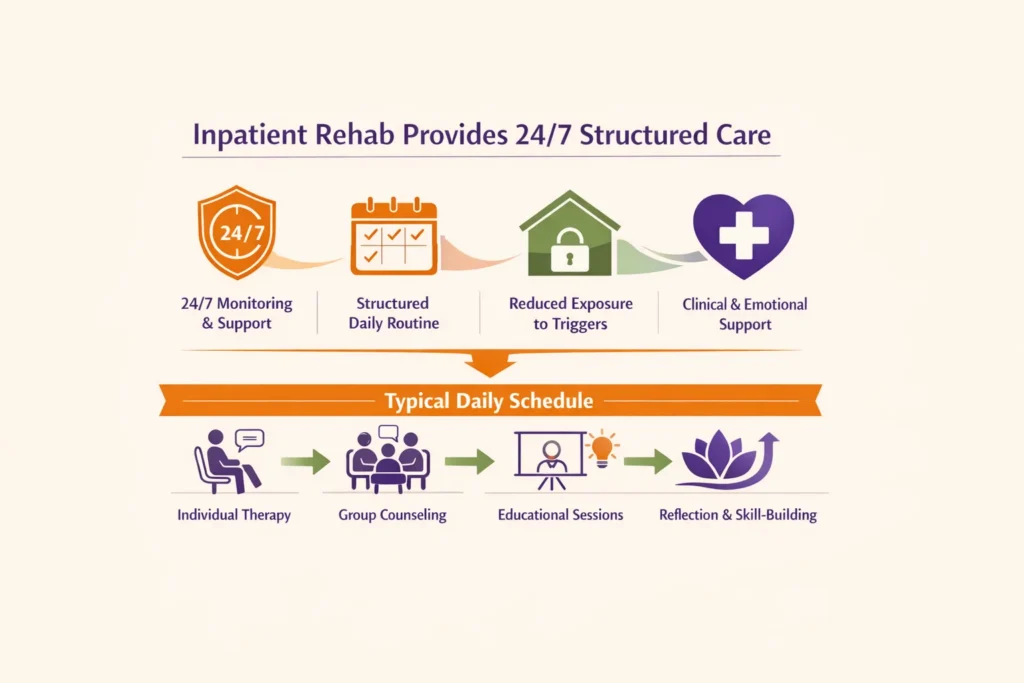
2. Inpatient Rehab Provides 24/7 Structured Care
Inpatient rehab programs provide a structured, live-in environment where individuals receive continuous care and supervision throughout the recovery process. This setting is designed to reduce exposure to external triggers while offering consistent clinical and emotional support. With 24/7 monitoring, individuals can focus fully on recovery in a stable and substance-free setting.
Daily schedules in inpatient rehab are typically organized and may include:
- Individual therapy sessions
- Group counseling and peer support
- Educational and recovery-focused activities
- Time for reflection and skill-building
This structured approach helps reinforce routine, accountability, and progress in early recovery.
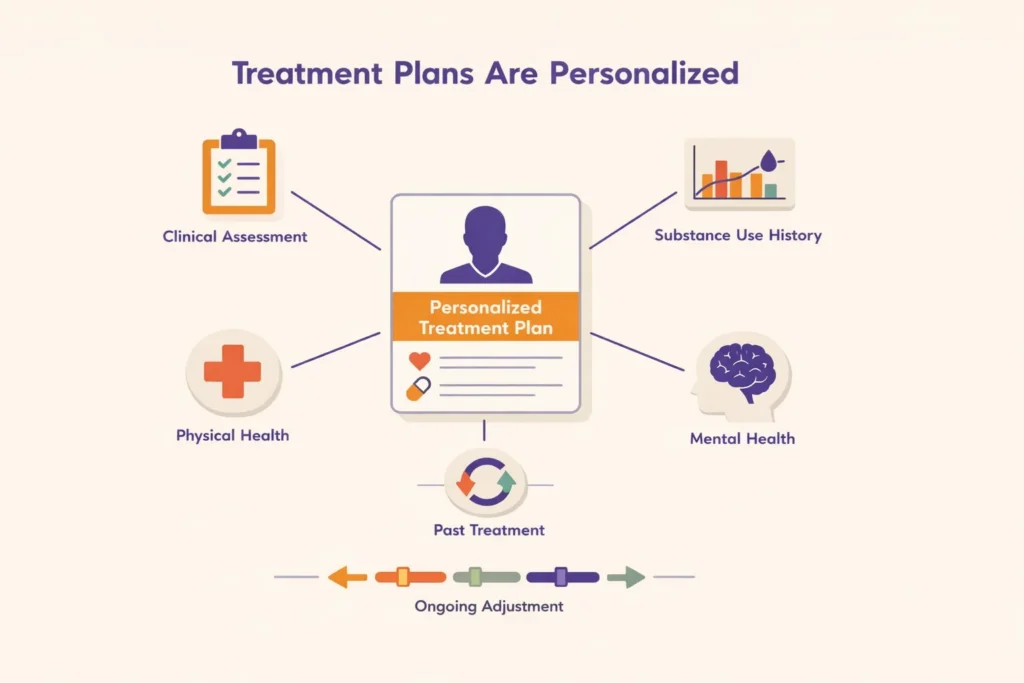
3. Treatment Plans Are Personalized
Inpatient detox and rehab programs use individualized treatment plans tailored to each person’s unique needs and circumstances. Rather than applying a one-size-fits-all approach, providers develop care plans based on a comprehensive clinical assessment and ongoing evaluation throughout treatment.
Several factors may influence how a treatment plan is structured, including:
- Severity and duration of substance use
- Physical health and medical history
- Mental health conditions
- Previous treatment experiences
This individualized planning allows providers to adjust care as treatment progresses, ensuring it remains responsive to changing needs.
4. Multiple Levels of Care May Be Involved
Inpatient detox and rehab are often part of a broader continuum of care, where individuals move through different levels of treatment based on their needs and progress. After completing inpatient care, many transition into less intensive programs that still provide structure and support.
This step-down model allows individuals to gradually regain independence while maintaining clinical guidance. For example, some may continue treatment through structured outpatient care, which offers ongoing therapy and support while allowing for greater flexibility in daily life.
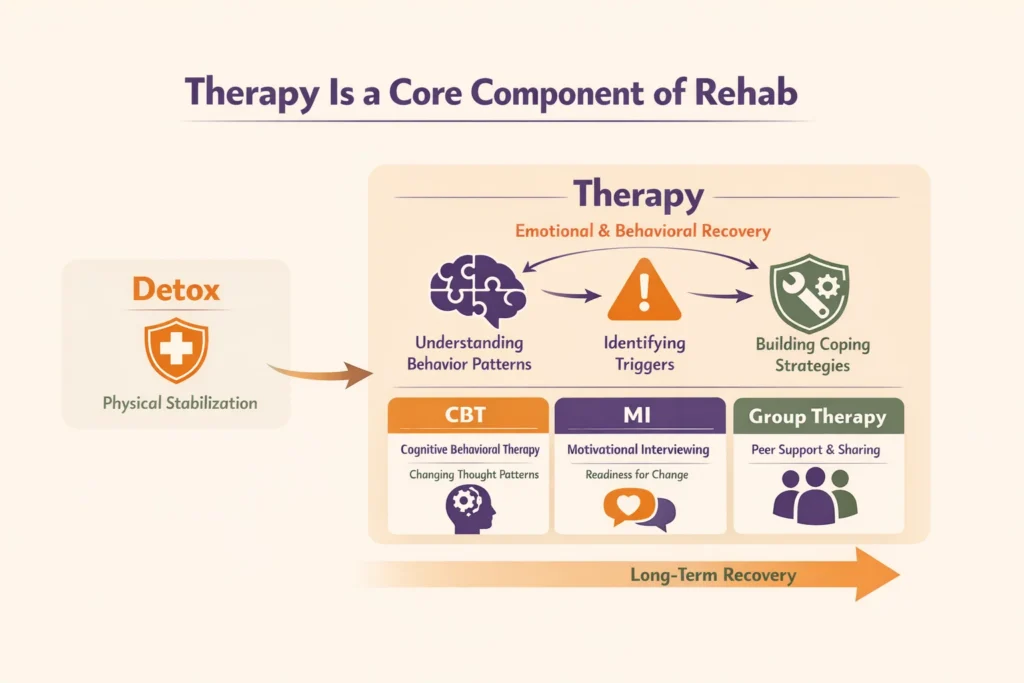
5. Therapy Is a Core Component of Rehab
Therapy is a central part of inpatient rehab, focusing on the behavioral and psychological factors associated with substance use. While detox addresses physical dependence, therapy helps individuals understand patterns of use, identify triggers, and develop healthier coping strategies that support long-term recovery.
Several evidence-based approaches are commonly used in treatment, including clinical guidelines for addiction treatment developed by the American Society of Addiction Medicine. Cognitive behavioral therapy (CBT) focuses on changing unhelpful thought patterns, while motivational interviewing (MI) helps strengthen a person’s readiness for change. Group therapy also plays an important role by providing peer support, shared experiences, and opportunities to build communication and interpersonal skills.
6. Co-Occurring Mental Health Conditions Are Often Treated
Some individuals experience both substance use and mental health conditions at the same time, a combination often referred to as dual diagnosis. These conditions may include anxiety, depression, trauma-related disorders, or other mental health concerns that can influence patterns of substance use.
Because these conditions often interact, integrated care approaches are commonly used in treatment settings. This means both substance use and mental health conditions are addressed together through coordinated therapy and clinical support. Many individuals benefit from dual diagnosis treatment programs, which are designed to provide comprehensive care within a single, structured setting.
7. Medications May Be Used to Support Recovery
In some cases, medications may be used as part of a comprehensive treatment plan to support recovery after detox. These medications are typically prescribed by licensed medical professionals and are used alongside therapy and behavioral support, rather than as a standalone solution.
Common examples include naltrexone, which may help reduce alcohol cravings, acamprosate, which supports continued abstinence, and disulfiram, which produces adverse effects if alcohol is consumed. These are among the medications used in the treatment of alcohol use disorder, with treatment decisions based on individual clinical needs.
8. Length of Stay Can Vary
The length of stay in inpatient detox and rehab can vary depending on individual needs and clinical recommendations. There is no fixed timeline, as treatment duration is based on a range of personal and medical factors.
Several factors may influence how long someone remains in treatment, including:
- Severity and duration of substance use
- Physical health and medical stability
- Presence of co-occurring mental health conditions
- Progress made during treatment
Because recovery is an ongoing process, length of stay is often adjusted to ensure individuals receive the appropriate level of care at each stage.
9. Support Systems Play an Important Role
Support systems play a critical role in maintaining recovery after inpatient detox and rehab. While clinical treatment provides a strong foundation, ongoing support can help reinforce stability and reduce the risk of relapse over time.
These support systems may include:
- Peer support groups and recovery communities
- Family involvement and counseling
- Sober living or structured environments
In Virginia, individuals may also access community-based resources, such as the Fairfax County Community Services Board’s substance use disorder programs, which offer local support services and continued care options. Together, these forms of support help individuals stay engaged in recovery beyond formal treatment.
10. Transition Planning Is Part of the Process
Transition planning is an important part of inpatient detox and rehab, helping individuals prepare for the next stage of recovery after completing a higher level of care. Before discharge, treatment providers typically develop a plan based on clinical progress and ongoing needs.
This process may include referrals to outpatient programs, therapy providers, or community-based support services. By ensuring continuity of care, transition planning helps reduce gaps in support and provides a structured path forward as individuals continue their recovery journey.
What to Expect From Inpatient Detox and Rehab in Virginia
Inpatient detox and rehab programs in Virginia are designed to provide a structured and comprehensive approach to recovery, beginning with physical stabilization and continuing through therapy and ongoing support. While detox helps manage withdrawal symptoms, long-term recovery typically involves addressing the behavioral, psychological, and environmental factors associated with substance use.
Because recovery needs vary, individuals may move through different levels of care over time, supported by therapy, structured programs, and community resources. This process is often tailored to each person’s circumstances, with adjustments made as treatment progresses.
Understanding how inpatient detox and rehab work can help individuals and families set realistic expectations and make informed decisions about the recovery journey.
Frequently Asked Questions
How is inpatient detox different from rehab?
Inpatient detox focuses on managing withdrawal symptoms and stabilizing the body, while rehab addresses the behavioral, psychological, and emotional factors associated with substance use. Detox is typically the first step, followed by structured treatment that supports long-term recovery.
Is inpatient rehab required after detox?
Inpatient rehab is not always required after detox, but many individuals benefit from continued structured care. The appropriate level of treatment is typically determined through a clinical assessment based on individual needs and circumstances.
How long does inpatient rehab last?
The length of inpatient rehab varies depending on factors such as substance use history, overall health, and progress during treatment. Some individuals may remain in treatment for several weeks, while others transition sooner to lower levels of care.
What happens after inpatient rehab?
After inpatient rehab, individuals often continue recovery through outpatient programs, therapy, or support groups. Ongoing care and support systems can help maintain progress and reduce the risk of relapse over time.








