Same-day rehab admission refers to an expedited process that allows individuals to enter treatment as quickly as possible, often within the same day of initial contact. While the term suggests immediate placement, the process is not instant. Admission still involves a structured clinical intake designed to ensure safety, accuracy, and appropriate care.
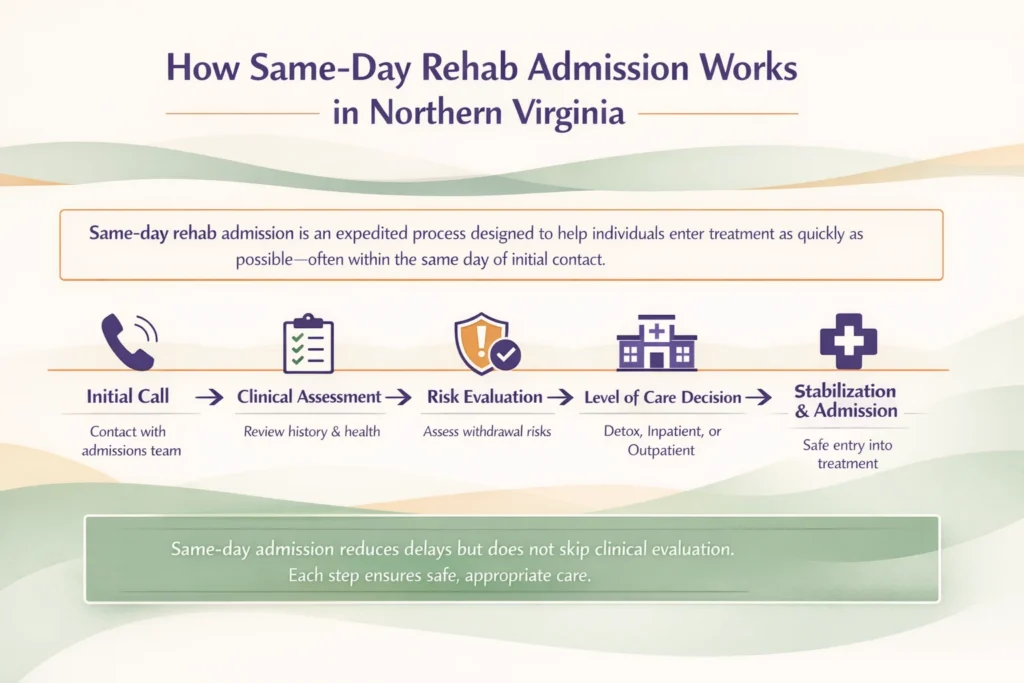
This process typically begins with an initial call, followed by a clinical assessment that reviews substance use history, mental health, medical needs, and potential withdrawal risk. These steps help determine the most appropriate level of care, whether that involves detox, inpatient treatment, or outpatient support.
Same-day admission focuses on reducing delays, not bypassing evaluation. Each stage, from assessment to stabilization and placement, is guided by clinical decision-making. Understanding how this process works can help set clear expectations and provide a more accurate picture of what happens when seeking immediate treatment.
What Same-Day Rehab Admission Means
Same-day rehab admission refers to an accelerated intake process designed to reduce the time between initial contact and entry into treatment. It allows individuals to begin care as quickly as possible, often within the same day, while still following a structured clinical evaluation.
This option typically applies in situations where there is an immediate need for support, such as increased substance use, withdrawal risk, or instability in daily functioning. However, availability does not always mean immediate placement. Admission depends on clinical appropriateness, which is determined through assessment rather than timing alone.
Clinical decision-making plays a central role in this process. Information gathered during intake helps determine whether same-day admission is suitable and what level of care is needed. The goal is not just speed, but ensuring that placement aligns with medical, psychological, and safety considerations.
When Immediate Rehab Admission May Be Recommended
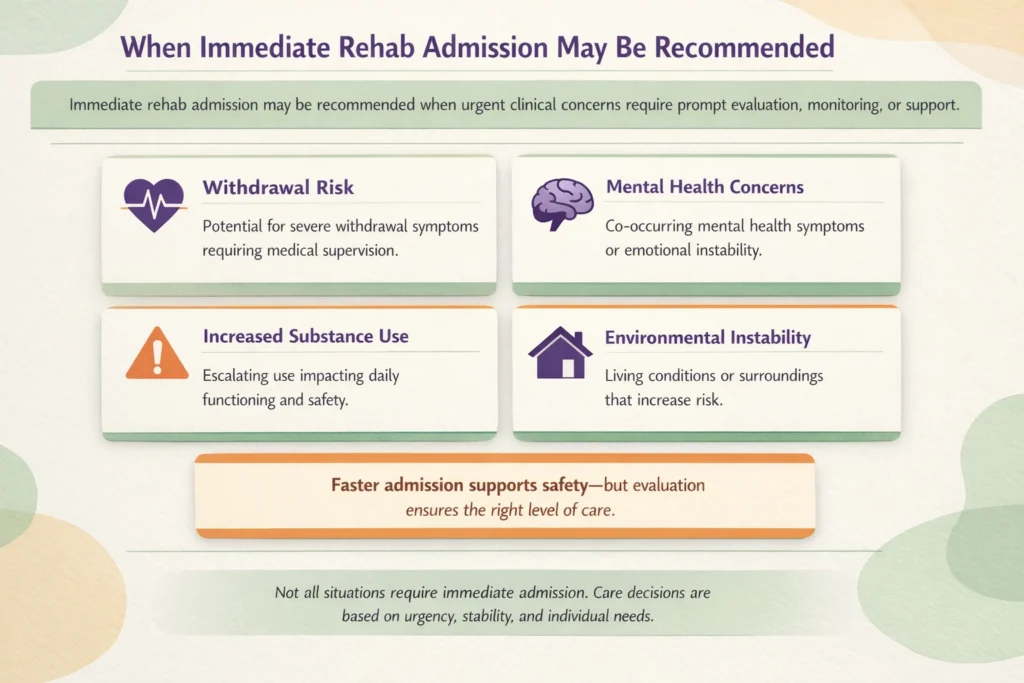
An accelerated admission process may be recommended when there are immediate clinical concerns that require prompt evaluation and support. One of the most common factors is the risk of withdrawal, particularly when symptoms could become severe or require medical monitoring. In these cases, reducing the time between assessment and care can be important for safety.
Other situations may involve mental health or environmental instability. This can include increased substance use, difficulty maintaining daily functioning, or conditions that raise concern for personal safety. These factors are evaluated together to determine whether a faster intake process is appropriate.
At the same time, immediate admission is not necessary in every case. Some individuals may be better suited for a planned start date based on their clinical presentation and support system. The decision is based on urgency, but also on ensuring that care aligns with current needs.
What Happens During the Initial Intake Call
The initial intake call is typically the first step in starting the admission process. It is designed to gather essential information and determine what type of care may be appropriate. In many cases, this call is available at any time, allowing individuals to begin the process without delay.
During the call, several key areas are reviewed. This includes substance use history, such as frequency, duration, and recent changes in use. Mental health symptoms are also discussed to identify any co-occurring conditions or concerns. Medical background, including current medications and past health issues, is considered to assess potential risks.
In addition to clinical details, the call often covers insurance verification and basic logistics, such as availability and timing. This helps clarify what options may be accessible. The information gathered during this step guides the next phase: a more comprehensive clinical assessment to determine the appropriate level of care.

Clinical Assessment and Placement Decisions
Following the initial intake, a comprehensive clinical assessment is completed to evaluate overall needs and determine the most appropriate next step. This process involves a more detailed review of substance use patterns, mental health history, and medical considerations.
One of the primary areas of focus is withdrawal risk. Certain substances can lead to symptoms that require medical supervision, making it important to assess severity, timing, and potential complications. When necessary, individuals may be referred to appropriate settings for safe stabilization before continuing treatment.
Mental health screening is also a key part of this evaluation, helping identify conditions that may influence treatment planning or require integrated support.
The information gathered during this assessment is used to guide placement into the appropriate level of care. This may include structured inpatient settings or outpatient options for those who can safely engage in care while maintaining daily responsibilities.
Placement decisions are based on clinical findings, with the goal of ensuring safety, stability, and continuity throughout the treatment process.
Levels of Care Available After Admission
Following admission, care is delivered across a range of levels based on individual clinical needs. These levels are designed to provide the appropriate structure, support, and monitoring as stability improves over time.
For individuals at risk of withdrawal, treatment may begin with medically supervised detox in a specialized setting. This allows for safe stabilization before transitioning into ongoing care. In cases where more structure is needed, inpatient treatment provides a highly supportive environment with continuous clinical oversight.
Partial hospitalization programs (PHP) offer a step down from inpatient care, combining structured daily support with the ability to begin integrating back into a more independent routine. This level of care often focuses on individualized planning, helping align treatment with each person’s specific needs, challenges, and goals as they move forward.
Each level of care functions as part of a continuum. Movement between levels is based on ongoing evaluation, ensuring that care remains aligned with changing clinical needs and overall progress.
What Happens in the First 24 Hours
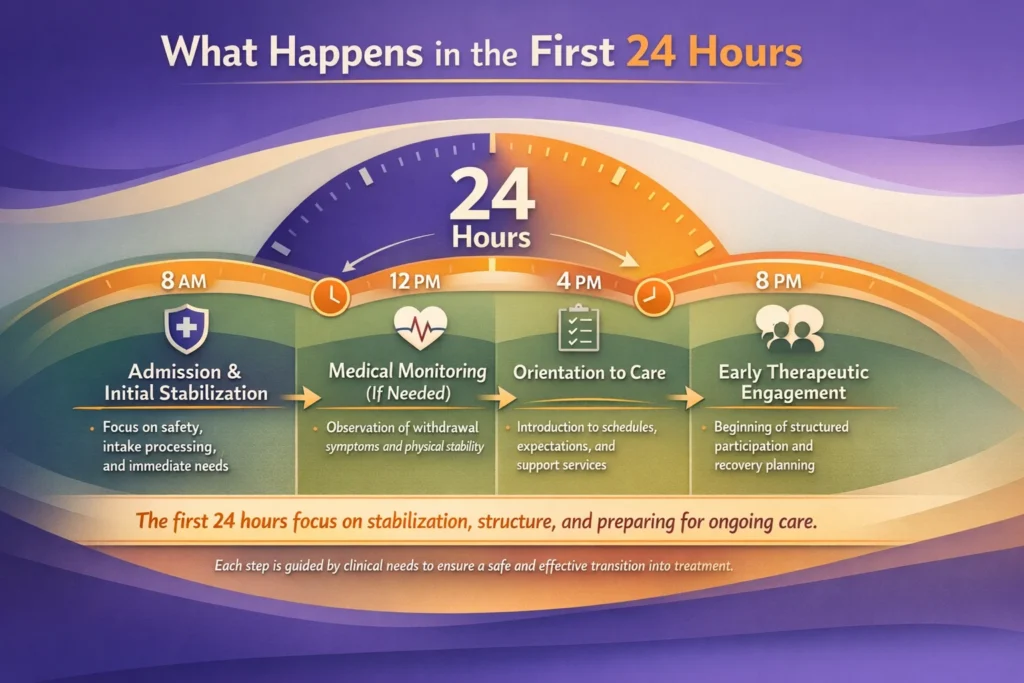
The first 24 hours after admission are focused on stabilization and orientation to care. During this period, initial steps are taken to ensure safety, establish structure, and begin the transition into a treatment setting.
For individuals with potential withdrawal risk, medical monitoring may be introduced as needed. This can involve observing symptoms, supporting physical stability, and determining whether additional medical oversight is required. The goal during this phase is to address any immediate concerns while preparing for ongoing care.
At the same time, orientation to the treatment process begins. This may include reviewing schedules, expectations, and an introduction to recovery support services in Virginia that may continue beyond the initial phase of care. Establishing a clear structure early on helps create consistency and reduce uncertainty.
The first day also marks the beginning of therapeutic engagement. While full programming may not start immediately, this period helps set the foundation for continued participation, with the focus on stability, clarity, and a structured path forward.
Factors That Affect Admission Timing
Several factors can influence how quickly admission can take place, even within an accelerated process. One of the most common considerations is availability. Openings within appropriate levels of care may vary depending on current capacity and clinical fit.
Insurance verification is another important step. Coverage, benefits, and authorization requirements can affect timing, particularly when additional approvals are needed before care begins. This process helps ensure that services are aligned with available resources.
Clinical appropriateness also plays a central role. The information gathered during intake and assessment must support a safe and effective placement, which may require coordination before admission can proceed.
Logistical factors, such as transportation and scheduling, can also impact timing. Together, these elements help set realistic expectations while ensuring that admission decisions remain focused on safety, accuracy, and continuity of care.
Accessing Same-Day Rehab Admission in Northern Virginia
Access to same-day rehab admission in Northern Virginia depends on a combination of availability, clinical readiness, and coordination across providers. While expedited intake options may be available, timing can vary based on current capacity and the level of care required.
The region includes a range of licensed treatment providers operating within established systems of care, including coordination across local health districts in Virginia.
Coordination between intake teams, clinical staff, and, when necessary, external providers plays a role in determining how quickly placement can occur. This structured approach supports both timely access and appropriate care, allowing individuals to begin treatment in a setting that aligns with their immediate needs.
What to Expect After Admission
After admission, the focus shifts toward integrating into a structured treatment environment. This includes following a consistent schedule, participating in clinical programming, and becoming familiar with the expectations of care. Establishing routine early on helps support stability and engagement.
Ongoing evaluation is a key part of this process. Clinical teams regularly review progress, monitor symptoms, and assess how individuals are responding to treatment. Adjustments may be made as needed to ensure that care remains aligned with current needs.
Movement between levels of care can occur over time based on this evaluation. As stability improves, individuals may transition into less intensive settings while continuing to receive support. This step-down approach allows care to adapt while maintaining continuity throughout the recovery process.
Long-Term Recovery After Immediate Admission
Entering treatment is an important first step, but recovery extends beyond the initial admission process. Long-term progress depends on consistency, structure, and continued engagement in care over time.
As individuals stabilize, the focus shifts toward maintaining progress through ongoing support. This often involves participating in step-down levels of care that provide continued structure while allowing for increased independence. Gradual transitions help reduce disruption and support sustained improvement.
Continuity of care plays a central role in this process. Ongoing evaluation, therapy, and support systems help reinforce skills developed during earlier stages of treatment. Recovery is not defined by how quickly someone enters care, but by the ability to maintain stability and adapt as needs change over time.
Frequently Asked Questions
How fast can you get into rehab?
In some cases, admission can begin the same day as the initial call. Timing depends on factors such as clinical needs, availability, and how quickly the intake and assessment process can be completed.
Is same-day admission guaranteed?
Same-day admission is not guaranteed. While the process can often be expedited, placement depends on clinical appropriateness, program availability, and any required coordination before care begins.
Do you always need detox first?
Detox is not required in every situation. It is typically recommended when there is a risk of withdrawal that may require medical supervision. A clinical assessment helps determine whether this step is necessary.
What should you bring?
Items may vary by program, but generally include identification, insurance information, prescribed medications, and essential personal belongings. Specific guidance is usually provided during the intake process to help prepare for admission.








